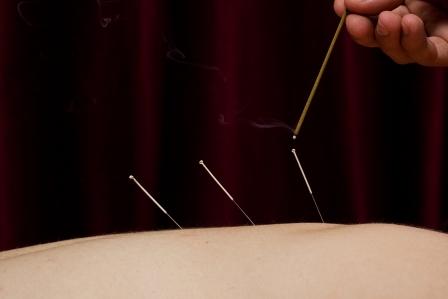
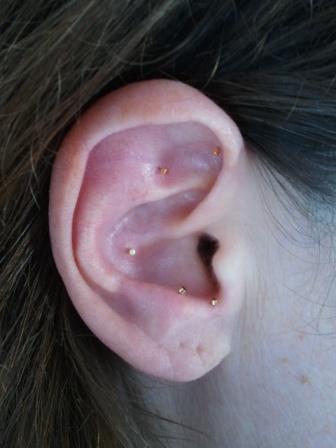
A guest post by an Acupuncture enthusiast
It is claimed that some studies in the use of acupuncture have shown that this therapy can be effective for reducing nausea and vomiting brought on by chemotherapy and after medical or dental operations. See www.ncbi.nih.gov/pubmed/10228456 and www.ncbi.nlm.nih.gov/pubmed/9809733 for example.
In addition advocates of acupuncture claim these trials also show that it may also be helpful in alleviating headaches, period pains, lower back pain and can help to ease the symptoms of addictions, osteoarthritis, tennis elbow, carpal tunnel syndrome and asthma among other conditions.
But are these so-called clinical trials valid? Below are a number of concerns raised by medical scientists and my response to these. At this point I will make it clear that I am not responding as a biomedical scientist. My response is based around how do you interpret what is truth?
Truth from the biomedical perspective of the scientist Robert T Carroll (see http://www.skeptic.com/acupunc.html) includes high calibre studies which should be “large, double-blinded, randomized, placebo-controlled clinical trials with low experimental attrition published in high quality medical journals that have been independently validated by other investigators.” (Bausell 2007)
Very few clinical trials on acupuncture fulfil any of these criteria. Carroll cites a number of examples of trials in which he points out that the number of participants were small; the drop-out rate was significant and the difference in variables between the acupuncture group, control group and the group following other medical advice too great to show valid and objective outcomes. These factors he points out skews the results in favour of acupuncture.
Unfair Clinical Trials for Acupuncture
For example in one study into whether acupuncture can help to improve cancer-related fatigue, the acupuncture group were given 20 minute sessions twice a week for three weeks. The acupressure group and sham acupressure group were taught to treat themselves by applying pressure to the real or fake points for one minute a day for two weeks.
The outcome of this trial was that the group who were treated with acupuncture reported the highest improvement rate to their fatigue.
Carroll rightly draws attention to two important facts. Firstly only the acupuncture group received treatment through direct administration by a therapist, the other two groups had to treat themselves. Many medical practitioners agree that patients are conditioned to expect improvement if they are treated directly by the therapist and that this is a significant contribution to the outcome of the treatment.
Secondly the length of time for the treatment between the acupuncture group and the other groups was hugely unequal. This was not a fair and objective clinical trial, therefore the validity of the results are highly dubious.
Fair point. In this case.
Let’s look at another example from a different medical source.
The clinical trial into the effectiveness of acupuncture in relieving post- operative or chemotherapy induced nausea has been highly criticised on www.acuwatch.org/general/nihcritique.shtml by Wallace I Sampson, MD, FACP.
A Biased Committee
He points out that most of the committee members who interpreted the findings of the trial were experts in social advocacy rather than in scientific thinking. He lists the members of the panel and their fields of expertise. The best qualified biomedical scientist, Dr Howard Fields, a pain physiologist from the University of California was absent from the trial due to illness. He did not agree with the committee’s findings. Furthermore most of the 16 page report on the findings of the trial was written before the conference.
In this case the interests of the group evaluating the trial were already biased in favour of acupuncture therefore their conclusions cannot be fair and objective.
This criticism into the validity of that clinical trial and others like it needs to be taken seriously. It is irresponsible to treat patients with methods of which the effectiveness is far from certain.
I shall return to the two criticisms above presently.
Other Problems with Assessing Acupuncture
There are other difficulties with assessing the effectiveness of acupuncture in clinical trials. Some of these are pointed out by NCAHF – the National Council Against Health Fraud – http://www.ncahf.org/
It is difficult to assess the difference between real acupuncturists and sham acupuncturists because there is a difference between the ability of genuine practitioners to locate acupunctural points based on experience. More experienced practitioners also disagree among themselves about the exact location of the points. Furthermore over 2,000 acupunctural points on the body have been identified by acupuncturists so it is highly likely that a sham acupuncturist will accidentally locate some of these points.
It is widely known that chronic pain is cyclic with periods of relief. Acute pain also becomes less intense over time without medical intervention. A patient reporting relief from acupuncture may be experiencing pain relief that would have happened naturally anyway.
Furthermore, as in any clinical trial, belief in the effectiveness of a placebo is enough to trigger physiological changes in the body such as the release of endorphins and adrenalin. Patients can also be conditioned to expect improvement to their symptoms within a medical setting by the presence of medical equipment, gowns worn, the jargon used by the professionals, the manner of the healer and may also feel better though the attention they are given or by the comfort of physical contact.
It is also argued that the kind of people who volunteer for clinical trials using acupuncture may be consciously or unconsciously biased in favour of this treatment and therefore more likely to report a favourable outcome including a false placebo effect.
Acupuncture is No Longer the Preferred Medical Treatment in China
The NCAHF points out that acupuncture as a method of treatment was actually banned in China in 1929. It enjoyed a renaissance when reinstated during Chairman Mao’s notorious Cultural Revolution during the 1960s as part of his propaganda to promote a re-born Communist China.
On www.skeptics.com Carroll voices the concern that popularist celebrity endorsements of alternative treatments seem to carry more weight in validating these treatments as more effective than “a thousand high-calibre scientific studies.”
This also includes inaccurate reporting of sensational news about the use of acupuncture. For example acupuncture rose in popularity in the West after it was reported in the New York Times that journalist James Reston underwent an appendectomy with only acupuncture used to control the pain. What actually happened was that the operation was performed using chemical anaesthetics and Reston was given acupuncture afterwards to relieve post-operative pain.
A Response to the Critique
Unfair clinical trials, biased interpretations of these, political propaganda and misreporting of actual events are serious concerns and undermine the credibility of acupuncture.
On the other hand why is there a lack of large high-calibre clinical trials in this area? Could it be to do with the inherent bias and/or political agenda of those responsible for funding these trials and is that why acupuncture trials are seldom reported in high quality scientific journals?
In the West the most dominant model of health is the biomedical model. “Health” is regarded primarily as the absence of disease, in other words health is defined primarily in terms of what it is not. (Source: Stephen Pattison, ‘Alive and Kicking’ SCM Press, London, 1989, Ch. 2, pp. 7 -20) Because health is viewed in terms of what it is not, treatment is usually placed into the hands of experts of scientific knowledge who intervene. The accepted process of intervention is mechanical and technical. Success can only be measured in empirical, verifiable results.
The inherent assumption here is that only technical difficulties lie between the eradication of the problem and full health. In practice this means that many human and financial resources are channelled into areas where there is already concentrated research. In the NHS for example the top priority of resources goes towards teaching hospitals and to treating acute illnesses where the outcome is easily measurable. It has been branded the National Hospital Service. (Gwyn Bevan, ‘The Structure of the National Health Service’ in N. Black et al., Health and Disease: A Reader p. 196)
Now at this point scientists and lay readers alike may think, “Hang on! Surely it is right to allocate most resources towards teaching and research into the advancement of new technology?” If the biomedical model of health was the only valid model of health then that would be true.
Truth however can be looked at from other perspectives. From an ethical perspective where the world has a finite bank of resources it has to be asked at what cost is funding being constantly allocated to ever evolving technical and chemical advancements? How environmentally sustainable is this in the long term? Is it not worth researching more natural and low-costing remedies such as acupuncture if there is a chance of proving that these are just as efficacious and have fewer side-effects?
From a humanist and social perspective what aspect of our healthcare is important? Whose health is important? The biomedical model of health focuses on the eradication of disease with success being defined as a complete cure. This is ultimately an impossible aim – we naturally weaken as we age and eventually die. So what kind of care do we give and receive for our well-being? It is well known that most serious illnesses can be prevented by acts of simple everyday care from washing hands after using the toilet to eating foods that are nourishing. In many parts of the world people do not have access to basic healthcare resources and in the UK several hospitals have come under severe criticism for the lack of nursing care and neglect of vulnerable patients such as the elderly.
So can the opinion of health professionals with a leaning towards social advocacy on the committee boards of clinical trials on acupuncture be dismissed as lacking credibility? Surely their presence is highly important to raise the outlook on healthcare from a microscopic level to the broader horizon of who can access this treatment and how sustainable is it in the long term?
And what of the other practical problems in accessing the true effectiveness of using acupuncture to alleviate headaches such as differentiating between real and sham acupuncture, the nature cycle that the intensity of pain follows, the influence of conditioning and so on? Those who are searching for evidence in support of acupuncture sometimes rely on the meta-analysis of several smaller trials. These are dismissed by sceptics such as Carroll as not being as reliable as large scale clinical trials because researchers are selective about which studies to include in their analysis. Yet if adequate funding is not allocated to larger studies in acupuncture then what other options do they have?
Perhaps other factors such as the placebo effect, natural progression of illness and pain and the conditioning of patients to expect an improvement would worry acupuncturists if they viewed their role through the lens of the medical model of health. Therapists in complementary medicine do not claim to be omniscient about an individual’s needs. The treatment of a person cannot be made in isolation from environmental and social factors because human beings by their nature are multi-dimensional, inter-relational and spiritual beings. The body is more than a machine that can be split into separate parts or systems and parcelled out to different specialists in different hospitals. The other factors in a patient’s perceived sense of recovery – which are incidentally just as relevant in using conventional Western medical treatment – can be welcomed as addressing the needs of the whole person.
What about the danger that if a patient believes – or politely says – they are feeling much better, that a serious underlying condition may be overlooked? Well, if the acupuncturist operated in a social vacuum that would be a real danger. Any responsible therapist would encourage their patients to take responsibility for their own healthcare as well and to make necessary lifestyle changes and seek scientific medical treatment if appropriate. Again, you have only to read the local newspapers to read of many cases of serious or life-threatening conditions being overlooked within hospitals due to understaffing or neglect or too many people using emergency services for the wrong reasons.
The NCAHF criticises acupuncture for being based on primitive concepts of health and disease. The idea of acupuncture points being used to stimulate the flow of Qi – the body’s flow of energy – is dismissed as fanciful nonsense because it cannot be proven that this mythical Qi actually exists. This is why the popularity of acupuncture in China has been supplanted by Western medicine it is claimed. What the NCAHF fails to point out is the sheer number of acupuncturists who show they are well-versed in their scientific understanding of how the body works on their websites and in publications. Practitioners seek to enhance that understanding by finding out how much the person is in balance with themselves and their environment. So-called “primitive knowledge” is experiential knowledge from a time when human beings lived less isolated lives and were much more in tune with their natural environment. We lose touch with that knowledge at our own long term cost.
As for the serious allegation that interest in acupuncture only revived in China due to Chairman Mao’s programme of propaganda, notice that nothing is said about the sudden suppression of acupuncture in 1929? Could the collapse of the ancient Chinese fief system and the unification of China under the Kuomintang regime have anything to do with it? In 1927 the capital was moved from Peking in the north not far from the borders of Mongolia where acupuncture originated to Nanjing in the South. The banning of acupuncture was part of a political programme designed to cement the unification process by eradicating examples of independent cultural heritage, particularly from the north. The provision of healthcare is always a big football for the politicians to play with in any society. Whether or not a particular regime endorses a particular form of treatment or not cannot be used to argue against the validity of acupuncture.
To conclude, it would seem that scientists are not unbiased and unprejudiced when it comes to encouraging research and analysing the findings of studies into acupuncture. There is evidence that the critics I have cited have been highly selective with presenting and interpreting their evidence against the validity of acupuncture. Acupuncture is not there to supplant the benefits of modern technology and advances in scientific knowledge. It is there to enhance people’s overall experience of healthcare.
Chrissy McAteer